Last Updated: May 28, 2026
Introduction to Hemochromatosis
Hemochromatosis is defined as a disorder in iron metabolism that is characterized by excess iron absorption, saturation of iron-binding proteins and deposition of hemosiderin (amorphous iron deposits) in the tissues. The primary affected tissues are the liver, pancreas, and skin. Iron deposition in the liver leads to cirrhosis and in the pancreas causes diabetes. The excess iron deposition leads to bronze pigmentation of the organs and skin. In fact, the bronze skin pigmentation seen in hemochromatosis, coupled with the resultant diabetes lead to the designation of this condition as bronze diabetes.
Primary Hemochromatosis
Primary hemochromatosis is an autosomal recessive disorder that is referred to as type 1 hemochromatosis. The locus causing type 1 hemochromatosis has been designated the HFE locus (homeostatic iron regulator) and is a major histocompatibility complex (MHC) class 1 gene.
Hemochromatosis, that is associated with the HFE locus, is one of the most commonly inherited genetic defects. Manifestation of the symptoms of the disease is modified by several environmental influences. Dietary iron intake and alcohol consumption are especially significant to hemochromatosis. Menstruation and pregnancy can also influence symptoms. Hemochromatosis occurs about 5 to 10 times more frequently in men than in women. Symptoms usually appear between the ages of 40 and 60 in about 70% of individuals.
Molecular Biology of Primary Hemochromatosis
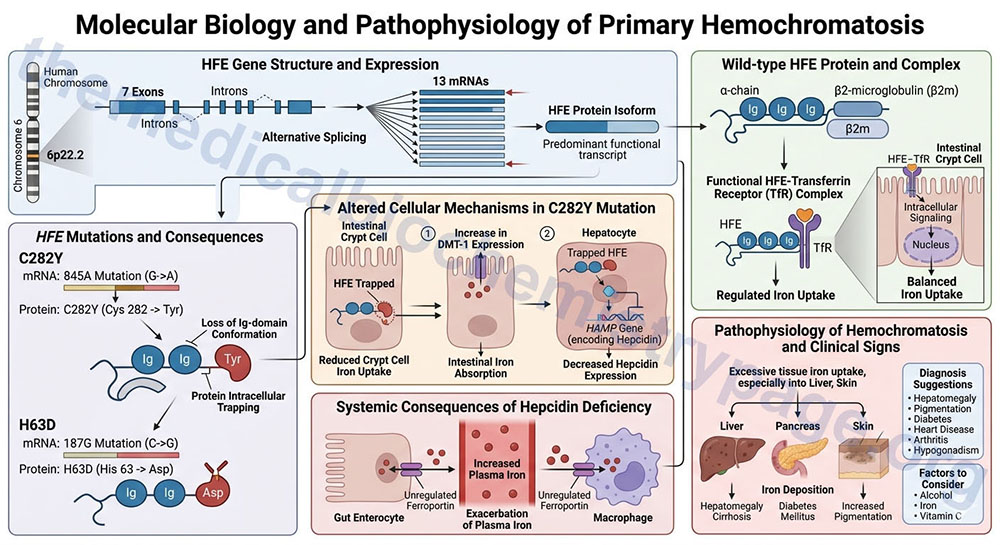
The HFE gene is located on chromosome 6p22.2 and is composed of 7 exons that generate 13 alternatively spliced mRNAs, each of which encode a distinct protein isoform.
The HFE gene encodes an α-chain protein with three immunoglobulin-like domains. This α chain protein associates with β2-microglobulin, typical of MHC class 1 encoded proteins. The normal HFE encoded protein has been shown to form a complex with the transferrin receptor and in so doing is thought to regulate the rate of iron transfer into cells. A mutation in HFE will therefore, lead to increased iron uptake and storage.
The majority of hereditary hemochromatosis patients have inherited a mutation in HFE that results in the substitution of Cys 282 for a Tyr (referred to as the C282Y allele). The C282Y allele results from a missense mutation of a G to an A at nucleotide 845 (termed the 845A mutation) of the HFE mRNA. This mutation causes loss of conformation of one of the immunoglobulin domains in the HFE encoded protein. Another mutation found in certain forms of hereditary hemochromatosis also affects the HFE gene and causes a change of His 63 to Asp (referred to as the H63D allele). The H63D allele results from a missense of a C to an G at nucleotide 187 (termed the 187G mutation) of the HFE mRNA. This latter mutation is found along with the more common C282Y mutation resulting in a compound heterozygosity. Of note, homozygosity for the H63D mutation is itself not associated with clinically significant iron overload.
As a result of the C282Y mutation the HFE protein remains trapped in the intracellular compartment. This trapping of HFE protein results in the interference of its role in transferrin receptor-mediated control of iron uptake by cells as well as its role in the regulated expression of the HAMP gene (encoding hepcidin). Because the HFE protein cannot associate with the transferrin receptor there is a reduced uptake of iron by intestinal crypt cells.
It is thought that this defect in intestinal iron-uptake results in an increase in the expression of the divalent metal transporter (DMT-1) on the brush border of the intestinal villus cells (for more information on iron uptake and transport see the Iron and Copper Homeostasis page). Excess DMT-1 expression leads to an inappropriate increase in intestinal iron absorption. Additionally, because HFE is trapped it cannot participate in the signaling cascade leading to activation of the HAMP gene.
Decreased expression of hepcidin leads to unregulated presentation of the iron transporter, ferroportin, in the basolateral membranes of intestinal enterocytes and in the plasma membranes of macrophages. With no control over iron release to the blood from these two cell types, there is an exacerbation of increased plasma iron. Since there is reduced to no HFE-mediated regulation of the transferrin receptor, too much iron is absorbed into tissues, particularly the liver, pancreas, and skin leading to the progressive symptoms of hemochromatosis.
Pathophysiology of Primary Hemochromatosis
In hemochromatosis the liver is usually the first organ to be affected. Hepatomegaly will be present in >95% of patients manifesting symptoms. Initial symptoms include weakness, abdominal pain, change in skin color and the onset of symptoms of diabetes mellitus. In advanced cases of hemochromatosis there will likely be cardiac arrhythmias, congestive heart failure, testicular atrophy, jaundice, increased pigmentation, spider angiomas and splenomegaly. Diagnosis of the disease is usually suggested when there is the presence of hepatomegaly, skin pigmentation, diabetes mellitus, heart disease, arthritis and hypogonadism. The degree of increase in total body iron stores in patients suspected of having hemochromatosis should focus primarily on parenchymal iron concentration. It is also important to ascertain whether other circumstances could be the cause of the symptoms of iron overload. These would include alcohol consumption, iron intake and excessive vitamin C ingestion as the latter promotes iron absorption.
Treatment of Primary Hemochromatosis
Treatment of hemochromatosis before there is permanent organ damage can restore life expectancy to normal. Treatment involves removal of the excess body iron. This is accomplished by twice-weekly phlebotomy at the beginning of treatment. Alcohol consumption should be curtailed and preferably eliminated in hemochromatosis patients. Iron chelating agents, such as deferoxamine, can be used to remove around 10 to 20 mg of iron per day. However, these agents are expensive and phlebotomy is more convenient and safer for most patients.
Non-HFE Hemochromatosis
There are several additional causes of hemochromatosis, although none are as common as classic hemochromatosis. There are at least four additional genetic loci, that when defective lead to hemochromatosis. Two of which are juvenile forms identified as type 2A and 2B and two additional forms identified type 3 and type 4.
Juvenile hemochromatosis (JH) type 2A
Juvenile hemochromatosis (JH) type 2A is the result of defects in the gene encoding hemojuvelin (HJV; formerly HFE2). This disorder is sometimes referred to as HFE2A. The function of hemojuvelin is to regulate the expression of the hepcidin gene (HAMP) via bone morphogenetic protein (BMP) signaling pathways.
As suggested by the juvenile nomenclature, this disorder manifests in patients under the age of 30. Cardiomyopathy and hypogonadism are prevalent symptoms with type 2A hemochromatosis. Type 2A hemochromatosis is inherited as an autosomal recessive disorder. The hemojuvelin protein is one of three members of a family of glycosylphosphatidylinositol (GPI)-linked cell membrane-associated proteins that were originally identified as repulsive guidance molecules, RGM. Hemojuvelin is also known as RGMc and is expressed predominantly in the liver and skeletal muscle. The other two members of the family, RGMa and RGMb, are predominantly expressed within the nervous system. RGMa is a repulsive guidance molecule for retinal axons and RGMb is involved in patterning of the central nervous system.
The HJV gene is located on chromosome 1q21.1 and is composed of 4 exons that generate six alternatively spliced mRNAs that collectively encode three distinct protein isoforms.
Juvenile hemochromatosis (JH) type 2B
JH type 2B results from defects in the gene encoding hepcidin (HAMP). This disorder is sometimes referred to as HFE2B. As with type 2A disease, symptoms of type 2B disease appear in patients under 30 years of age and include cardiomyopathy and hypogonadism. Type 2B hemochromatosis is inherited as an autosomal recessive disorder.
Hepcidin was initially described as a 25 amino acid peptide resembling cysteine-rich antimicrobial peptides. Recent evidence has demonstrated that hepcidin functions by inhibiting the presentation of one or more of the iron transporters (e.g. DMT1 and ferroportin) in intestinal membranes. With a high iron diet the level of hepcidin mRNA increases and conversely its levels decrease when dietary iron is low. See the Iron and Copper Homeostasis page for more information of iron transport.
The HAMP gene is located on chromosome 19q13.12 and is composed of 3 exons that encode an 84 amino acid preproprotein.
Type 3 hemochromatosis
Type 3 hemochromatosis is caused by mutations in the gene (TFR2) encoding transferrin receptor-2. This disorder is sometimes referred to as HFE3. TFR2 is a homolog of the classic transferrin receptor (identified as TFR1) which is responsible for the uptake, into cells, of transferrin-bound iron (see the Iron and Copper Homeostasis page for more information on iron transport).
Unlike the ubiquitous expression of TFR1, TFR2 expression is almost exclusively found in the liver. The function of TFR2 in the liver is not to act in the uptake of transferrin-bound iron but to sense iron levels and to act as a regulator of hepcidin function. The clinical features of type 3 hemochromatosis are similar to those of classic type 1 disease. Type 3 hemochromatosis is inherited as an autosomal recessive disorder.
The TFR2 gene is located on chromosome 7q22.1 and is composed of 18 exons that generate two alternatively spliced mRNAs, both of which encode distinct protein isoforms.
Type 4 hemochromatosis
Type 4 hemochromatosis is also called ferroportin disease because it is caused by mutations in the gene (SLC40A1) that encodes the ferroportin protein. Type 4 hemochromatosis is also sometimes referred to as HFE4.
The protein encoded by the SLC40A1 gene is also identified as IREG1 (iron-regulated transporter 1) and MTP1 (reticuloendothelial metal transporter 1). SLC40A1 was also known as SLC11A3 but this latter designation is no longer used.
Ferroportin is a multiple transmembrane-domain containing iron transport protein. It is highly expressed in the liver, duodenum, and on reticuloendothelial cells. The major function of ferroportin is to transport dietary iron across the basolateral membranes of intestinal enterocytes into the blood and to recycle iron via the reticuloendothelial system. Symptoms of type 4 hemochromatosis are similar to those of classic type 1 disease but are generally milder. The unique aspect of type 4 hemochromatosis is that it is inherited as an autosomal dominant disease.
The SLC40A1 gene is located on chromosome 2q32.2 and is composed of 9 exons that encode a 571 amino acid protein.